The randomization was at the level of the EMS agency. This is a three-arm, pilot, cluster randomized trial with crossover conducted in 4 EMS services in Ontario, Canada. DOuble Sequential External Defibrillation for Refractory Ventricular Fibrillation: The DOSE VF Pilot Randomized Controlled Trial. The paperĬheskes S, Dorian P, Feldman M, et al. (Mapp 2019 Emmerson 2017 Cheskes 2019) However, we now have the first proper randomized trial looking at the practice, and the results aren’t bad. (By that logic, I am sort of surprised that no one has moved on to triple sequential defibrillation yet, but there is still time.) There has never been great evidence for the practice, and actually some observational data suggesting it might not be helpful. * Secondary Outcomes: Termination of ventricular fibrillation,Ĭopyright © The Skeptics Guide to Emergency Medicine 2012Double sequential defibrillation has been all the rage over the last few years in emergency medicine. * Primary Outcome: Survival to hospital discharge * Comparison: Standard defibrillation with pads placed in anterior-anterior configuration * Double Sequential External Defibrillation: Pads are placed in both the anterior-anterior and the anterior-posterior pad placements following the third shock with standard defibrillation. * Vector Change Defibrillation: Pads are placed in an anterior-posterior pad placement after standard anterior-anterior configuration following the third shock with standard defibrillation. * Population: Ontario patients who were at least 18 years of age and had an OHCA and refractory ventricular fibrillation. Defibrillation Strategies for Refractory Ventricular Fibrillation. One issue that has not been covered on the SGEM is pad placement and double sequential external defibrillation.Ĭlinical Question: Does refractory ventricular fibrillation respond better to standard defibrillation, vector-change defibrillation, or double sequential external defibrillation? 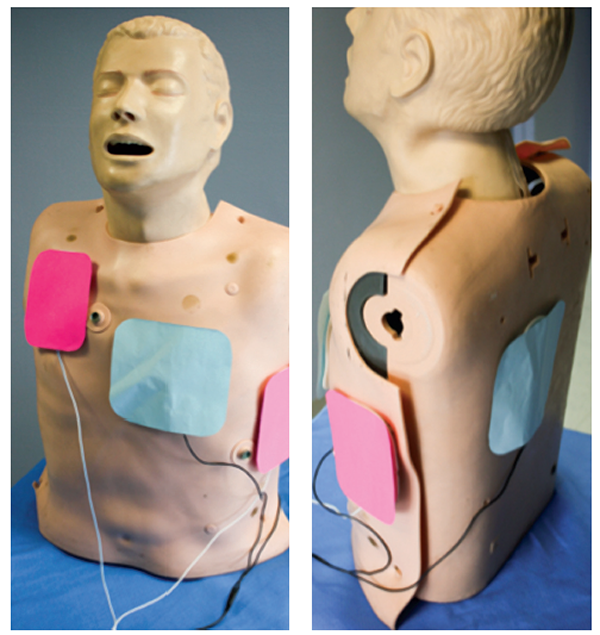
This has included things like therapeutic hypothermia (SGEM#54, SGEM#82, SGEM#183 and SGEM#275), supraglottic devices (SGEM#247), crowd sourcing CPR (SGEM#143 and SGEM#306), epinephrine (SGEM#238) and IO vs IV (SGEM#231 and SGEM#340). He arrives at the hospital 18 minutes into his arrest and his monitor shows persistent ventricular fibrillation.īackground: Out-of-hospital cardiac arrest (OHCA) is something we have covered extensively on the SGEM over the years. He is found to be in ventricular fibrillation and receives two defibrillation attempts with an automatic external defibrillator (AED) at the clinic, and subsequently three more with a primary care ambulance crew enroute to the hospital. He confirms pulselessness, initiates CPR, gets a colleague to call 911, and intubates the patient on the floor. An anesthetist is working with him for the procedures. He has been an ACLS instructor for close to 30 years and notably his first publication focused on out-of-hospital defibrillation.Ĭase: A 60-year-old health professional suffers a cardiac arrest while working at a clinic outside the hospital. He is an assistant professor at the Northern Ontario School of Medicine University and is passionate about health equity for rural and indigenous populations. Research interests include simulation-based assessment, transport medicine, and critical care analgesia. Guest Skeptic: Dr. Sean Moore is an emergency physician working in Kenora Ontario, where he is Chief of Staff at Lake of the Woods District Hospital, Northern Medical Director for the Ornge air medical transport program and associate medical director with CritiCall Ontario. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
